Please tweet and retweet
Tweet
Inflammation of the armpit glands or #Hidradenitis, was first described by Velpeau in 1839. In 1854, Verneuitt suggested that this condition might arise from the sweat glands of the skin and described the clinical condition which is now recognized as hidradenitis suppuritiva. Since then, hidradenitis surgeons have recommended many forms of treatment for this entity: lotions, vaccines, fever therapy, toxoids, steroids, ultraviolet light, X-rays, antibiotics, and surgery. The disease does not occur before puberty because the apocrine sweat glands do not function at that age. Patients see this as boils under the armpits that swell, drain foul smelling material and then swell again as the cycle starts over again.
The skin contains two types of sweat glands, the eccrine and the apocrine. The eccrine glands are distributed over the entire body's skin surface. The apocrine are found only in the armpits, groin, anal and pubic areas and the crease under the breast. Apocrine glands are 1arger than eccrine, are located more deeply in the skin and are derived from hair follicles. They do not function until the age of puberty. In lower animal forms the apocrines are a scent gland of sexual function. Apocrine glands are more numerous in females and in Afro-Americans. Consequently the female incidence of HS is greater than the male incidence. Apocrine sweat secretion contains part of the gland itself while eccrine sweat glands produce a water like secretion without any disruption of the gland.
Hidradenitis is not caused by deodorants, antiperspirants, cosmetics or hair removal creams/procedures. Obesity and/or smoking may aggravate the condition but are not a direct cause of hidradenitis. Usually, a plug of dead skin in the duct of a gland emptying into a hair follicle initiates the infectious process as bacteria multiply within the plugged gland. As the armpit gland swells a boil is seen under the armpit. The obstructed gland or boil ruptures into the deep layers of the skin; adjacent glands become involved; and abscesses form. Subsequently, multiple draining sinuses or holes appear on the skin surface and the whole hair bearing area may become inflamed. Such inflammation may result in star shaped skin scars and tunneling, causing ridging of the skin. The sinus tracts are considered the hallmark sign of hidradenitis. Another interesting finding has been the armpit and groin hair follicles are wider and deeper in hidradenitis although the exact cause and implications of this finding are unknown. My personal opinion is that friction between 2 skin surfaces or buttock and chair incite an inflammatory response against apocrine glands in susceptible individuals and it is this inflammation that results in infections and what we see as hidradenitis.
Deep-tissue samples of HS consistently demonstrate coagulase-negative staphylococci, a commensal organism usually find living on human skin. Because there is usually no true spread of infection with pathologic bacteria not normally found on the skin, even severe cases almost never result in fever, sepsis, or swollen lymph nodes and chronic use of antibiotics should be avoided.
 In this case of Hidradenitis of the armpit of many years duration multiple draining sinuses or holes on the skin surface, star shaped skin scars and tunneling causing ridging of the skin are easily seen.
In this case of Hidradenitis of the armpit of many years duration multiple draining sinuses or holes on the skin surface, star shaped skin scars and tunneling causing ridging of the skin are easily seen.This chronic localized skin infection usually continues for years with periodic remissions resulting in reclusive behavior, diminished ability to exercise and multiple days of work lost over time. The problem is these specific glands, the material they secrete and the way in which they secrete it. The disease is most common in the second and third decades of life and is three times more common in women. It's prevalence among women is 137 per 100,000 versus 58 per 100,000 men. Groin genitofemoral hidradenitis is significantly more common in women than in men. Armpit involvement is equal in both sexes. Patients with hidradenitis have more relatives with the disease than patients without hidradenitis although an exact chromosome carrying the disease has never been identified. Only rarely is hidradenitis controlled or cured with medications alone. The treatment for active infection is incision with drainage of the pus. The cure is to cut out all sources of infection and closure of the resulting wounds directly or with skin grafts or preferably skin flaps while the process is in a quiescent phase. The best appearing results are after direct or skin flap closure. Hence the need for a plastic surgeon.
When those sources of infection are removed they cannot cause any future problems. However, glands that have not been problematic to that point in time may become so at a future date. Although that is a theoretical possibility I have not seen that happen in my patient population. The most common problem I see after surgery is some separation of the suture line days to weeks after surgery. This is due to the tension of closure and the condition of the skin, which prolongs the healing process. In all cases these small separations have healed without any further problems. To decrease the risk of this happening and make any such separations smaller I place a few mattress sutures which approximate the skin edges without applying any tension to the edges.
Ignoring the disease or avoiding treatment is not a good idea because the disease is associated with a number of complications:
- Decreased range of motion due to scarring, especially in the armpits]
- Anal fistulas from hidradenitis around the anus
- Enlargement and distortion of the external genitalia
- Foreskin ulceratiions or destruction
- Anemia
- Low blood protein levels
- Squamous cell carcinoma, especially around the anus
TREATMENT
Treatment should take account of the phase in which the process is observed. In the initial stages, corticosteroid preparations are useful. During acute flare ups with draining pus incisions are made to ensure all of the pus is removed and the patient is given antibiotics, Rifampin together with clindamycin have worked well. You cannot removed the infected skin during these flare ups because you will not be able to suture the cut edges together in this infected environment. Vitamin A related medications like Accutane commonly used to treat acne have been prescribed but large cases series suggest that less than 25% of hidredenitis patients respond to such treatment.
When the chronic phase with sinuses is present only surgery by a hidradenitis surgeon will be effective. The operative treatment should consist of complete surgical removal of the involved area. Closure should preferably be with local flaps of skin. Free skin grafts are useful in certain cases.
 If you just cut out the hidradenitis and try to suture the wound closed the edges may not meet with larger excisions and if they do meet the resulting scar and skin loss usually restricts arm movement.
If you just cut out the hidradenitis and try to suture the wound closed the edges may not meet with larger excisions and if they do meet the resulting scar and skin loss usually restricts arm movement.Historically the remaining wounds were aloud to hear on their own which took months. A period of wound closure with skin grafts followed but only one armpit could have surgery at a time, the grafted armpit had to be immobilized with an airplane splint holding the arm out to the side for 2 weeks and the act of obtaining the skin graft created a remote area of skin scar elsewhere on the body. Also the skin grafted area is a different color than surrounding skin and lies in an indented area so the result is less aesthetic than skin flap procedures.

With improvements in plastic surgery techniques in the 1950s and 1960s a switch from skin grafts to skin flaps for closure after excision took place. The initial flaps used for this came with their own set of drawbacks. They were quite large and required skin grafts to close the area where the flap came from.

Then came skin flaps that were designed in such a way that skin grafts were no longer needed.


Then it became common knowledge that it was better to have 2 smaller flaps than one large one as that kept the scar confined within the armpit, still allowed closure without skin grafts, had a quick recovery without the need for splints, allowed a quick return to work, maintained arm range of motion and could be performed as outpatient surgery all without compromising the amount of armpit tissue that could be removed.

CASES

For more extensive disease the hole after removal is so great that I can only close it by moving a flap of skin from the back into the armpit area. In this case the after photo was taken 10 years after surgery without any recurrence of hidradenitis in that 10 year period.
For less severe cases or those who have surgery earlier I prefer 2 opposing V to Y advancement flaps of skin.

In this case the surgery was performed while the hidradenitis was in a quiescent phase so the armpit in the before surgery photo does not look so bad but it looks much worse when the disease is active and there is pus draining out of the skin sinuses. The surgery is considered successful because she no longer has active periods with draining pus and she has retained full range of motion. The cosmetic look of the armpit after surgery vs. during the quiescent phase before surgery is not a factor here.
The flap techniques used by plastic surgeons to close these wounds are based on the same principles we use to perform facelifts and tummy tucks. In those cosmetic procedures we take out the excess skin and close the wound with flaps of skin. In this case we take out the hidradenitis and then close the wound with skin flaps of skin.
Hidradenitis can occur around the anus in which case one needs to make sure there is no anal fistula or perirectal abscess before proceeding with surgery.
February 17, 2016 Addendum:
Danish researchers just published the analysis of a review of the Danish National Patient Registry, identifying 5,964 cases and 29,404 controls. They found an elevated risk of adverse cardiovascular (CV) outcomes, including death among patients with the inflammatory skin disorder hidradenitis suppurativa. Compared with healthy controls, the unadjusted incidence rate ratios among patients with hidradenitis suppurativa were:
- 2.18 (95% CI 1.61-2.94) for myocardial infarction,
- 1.73 (95% CI 1.32-2.25) for ischemic stroke, and
- 2.07 (95% CI 1.73-2.48) for the composite endpoint of major adverse cardiovascular events (P<0 .001="" all="" for="" li="">
- 2.54 (95% CI 1.87-3.44) for CV-associated death and
- 1.96 (95% CI 1.68-2.29) for all-cause mortality (P<0 .001="" both="" for="" li="">
That means someone with HS is at twice the risk of having a heart attack and 2 ½ times more likely to die from a cardiovascular incident than someone without HS.
The cause is believed to be high levels of systemic inflammation. They concluded that HS should be taken seriously and these patients need physicians who can manage them holistically.
Hidradenitis of the Breasts
Surgical Treatment of Hidradenitis
Bandages and Dressings for Hidradenitis Suppuritiva
Aaron Stone MD - Plastic Surgeon Los Angeles
Aaron Stone MD - twitter


i have a question about hidradenits i'm 14 and ma dad has this and i was wondering if you die from this stuff and if so how long do you have to live before you die from it? i have asked my dads doctor a bunch of questions but i have yet to get answer i understand please answer as soon as you can thank you
ReplyDeleteI have never heard of anyone dying from hidradenitis. It is not a fatal disease.
ReplyDeleteI've dealt with this disease for 15 years now. I am now 12 days post sweat gland removal and breast reduction for this disease. I was just wondering my arm is open im doing wet to dry and my skin graft scheduled Feb 3rd. I was wondering I have horrible headaches and neck pain could that be stress from my body and how im holding my posture?
DeleteOur physician said that infection occurring with hydradenitis may result in death.
ReplyDeleteAny infection can kill you if it is severe enough involving internal organs. Hidradenitis bothers patients so much with pain and drainage etc. that they usually seek medical attention before it becomes that severe.
ReplyDeleteHello! My sister has this disease and I was just wondering if after the skin flapping is finished, and the wound is healed, is the surgery noticeable? Will it always look as if she has gotten work done under her armpits? Also, is this same skin flapping procedure done with the breast area?
ReplyDeleteAll surgical incisions leave scars whose final appearance/visibility can take months to become clear. Non-pathological scars in this area is a very fair trade vs. constant oozing and pain from an area afflicted with hidradenitis.
ReplyDeleteHi does the major insurance cover this done by a plastic surgeon?
ReplyDeleteYes all major, government sponsored (Medicare), etc health insurance should cover this surgery even if it is performed by a Plastic Surgeon.
ReplyDeleteWhen you have the surgery to your goin area do you have to use skin grafts? I need to have this surgery and my doctor is sending me to see a general surgeon, should a plastic surgeon be seen instead?
ReplyDeleteSometimes you have to use skin grafts but the look is not as good and the recovery is longer than if you can use skin flaps from the abdomen or thighs. That is why you should see a plastic surgeon before having the surgery.
ReplyDeleteI have this disease and on oct 27th 2011 i had my surgery under both arms. Now both arms have opened back up and my plastic surgeon keeps saying that its healing but my physician said it is not because it is to open nd seems that some muscle is showing so i may need a skin graft. How long is the recovery for skin grafting and why do you think it opened back up and is not healing? Do you think i waited to long to check with my physician for a second opinion? I just wonder if im damaged even more.
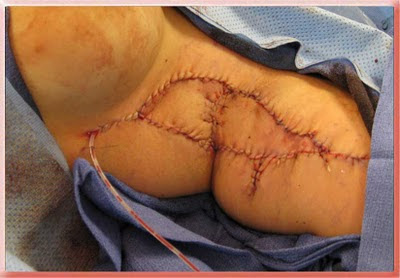
ReplyDeleteSkin closure after hidradenitis excision is notorious for splitting open due to the nature of the disease, motion of skin in the area and general condition of the skin. That is why I leave the sutures in longer than I normally would and add a few additional large sutures that enter and exit the skin some distance from the suture line (retention sutures). In the second photo from the bottom you can see the suture lines and the retention sutures used along where the bases of the 2 triangles of skin meet. Residual disease that was not removed at surgery can also cause the skin closure line to disrupt. Very rarely healed skin closure lines can reopen because of poor nutrition.
ReplyDeleteSkin grafting requires a 2 to 3 week healing process after surgery with activity restrictions to ensure that the skin grafts take - survive.
Hi
ReplyDeleteI just recently had surgery due to hidradenitis. Ive had a history with abscesses under my arm. I just wanted to know if my general surgeon using dermabond instead of sutures Was the right decision.
Not knowing exactly what was done or what your condition was I cannot say whether or not it was the right decision.
ReplyDeleteHi, I don't believe I have hidranetis but I am sure that I have some sort of an infection within my axilla. About 5 months ago, I tried to remove some hair within the armpit and I accidentaly left it on too long. A portion of the skin was pink immediately. I cleaned the area immediately and applied Neosporin the next morning. I was then put on a course of antibiotics as the axillary area began to get inflamed. I was advised by a dermatologist to not use deoderants for a while but rather a crystal rock deoderant. About one month ago, I began to use Certain Dri Deoderant when things started to look better, but within days, the axilla, and my whole arm became inflamed (including my palms/digits). I immediately discontinued usage and have been without deoderant for quite some time. The area around my axilla and the armpit skin has become quite sensitive as a result though and I always feel the need to itch. I'm not sure if my sensitivity in this region has increased. If it has, will it be permanent? I am currently at home wearing sleeveless clothing but in my current job, I can't continue to do so. Is it possible the area will not be as sensitive any more? I also feel a lot of tenderness in the surrounding arms and back as well. My blood tests are completely normal and they don't show any signs of an infection.
ReplyDeleteThanks for any advice.
This does not sound like hidradenitis because this temporarily affected you whole arm including the hand and fingers. You need to see a doctor face to face for an examination and diagnosis. Once the diagnosis is made a treatment plan can be worked out.
ReplyDeleteHi,
ReplyDeleteI have a consultation with a plastic surgeon coming up and Im very nervous about having this procedure. I spent years being misdiagnosed and taking antibiotics that didn't help. I have the condition under my armpits. How long would I expect to be restricted to do my daily activities? I have a 11 month old son and am worried about being able to care for him without interfering with the healing process. Can you give any advice or recommend anything for someone who has yet to have the procedure done?
Since I do not know your exact condition or exactly what procedure you are going to have I cannot make any recommendations regarding what you should do after surgery. If you have to use your arms to take care of your son it might be a good a idea to only do one armpit surgery and do the other armpit after you have fully recovered from the first surgery.
ReplyDeleteHi, thanks for the response. I have been researching into HS and I don't believe I have it. I have been to my GP as well as a Dermatologist he suggested. My GP has said that it is more than likely not HS. I did not know about HS when I spoke to the Dermatologist. The dermatologist said that I did not handle the situation well when I had the injury with the Depilatory Cream. As I put a spray on Deoderant 3 days afterwards. The inflammation is better but it varies and can sometimes come back. I am a little bit restricted in motion on both armpits. Are there any ways I could have samples of the skin tested, or perhaps I should request to see a particular type of doctor who would specialize in these type of dermopathologies. I am really committed to fixing this issue as it has affected me to a great extent. There is always a particular spot (where the injury occurred) on each armpit as well as near the lateral border of the axilla. I just want a sure way to make sure that this problem is not something serious that is not manifesting itself in a severe form. Are there any type of such tests that will help me rule out this possibility? I was concerned that it was a beginning stage of HS, but I don't believe that to be the case and I have also noticed that I have an odor that comes from me (very cheese like in smell) after I shower immediately afterwards.
ReplyDeleteNever having seen or examined you I have no idea what your diagnosis is. The diagnosis of HS is not a definitive one like a skin cancer or colon cancer. It is a clinical diagnosis where the history, physical examination and even the pathology of the excised tissue is said to be "consistent with hidradenitis suppuritiva".
ReplyDeleteI will be having surgery on my armpits and groin next week. Everyone says I should do everything at once and get it over with. My Dr would prefer I do one arm and one side of my groin then return for the rest. I'm terrified of the healing process. I don't want to do one side and be in so much pain I fear going back. Please advise if I should do it all at once or twice. My biggest concern is will I be able to walk while I'm healing if I do both sides of my groin.
ReplyDeleteNot knowing on the severity of your case or the specifics of the planned surgery I cannot say what would be best in your case. In general I prefer to operate on all areas at the same time unless the disease is quite extensive and I will need large rotation flaps for closure.
ReplyDeleteI recently went to my doctor who originally suggested I do a procedure called Isotretinoin (Accutane) for my condition under my armpits but discovered that my insurance wouldn’t cover it so now surgery is the next step. I recently just started a new job as a customer service rep where I sit and take calls all day. Is this something I would possibly still be able to do during my healing time for surgery or would complete bed rest the best way to heal??
ReplyDeleteI have never heard of using Accutane for hidradenitis and am pretty sure it will not work. Furthermore its use is restricted by law in the US.
ReplyDeleteYou would likely need to take some days off work after surgery after which you should be able to return with little or no restrictions especially since your work does not involve heavy manual labor.
Hi, I recently had skin graft surgery on April 24, 2012 and as of yesterday, May 14, 2012, the plastic surgeon has stated that the area doesn't seem to be healing as fast. My visit on April 30, the arm was 85% healed. However, my visit on May 7, he states that it is 65% healed. On my visit on May 14, he tells me that the area doesn't look any different than the week before. He said that the reason being is that it may be infected, and has referred me to a doctor who specializes in diseases and infections. I'm starting to lose confidence in him. What should I do?
ReplyDeleteNever having seen you and not knowing exactly what was done I cannot make any specific recommendations. Infections during recovery from surgery are not uncommon in these cases because of the nature of the disease. That can happen whether a skin graft or a flap is used. However, due to the limited blood supply in skin grafts vs. flaps the skin grafts have less resistance to infection. Generally these infections clear up with antibiotics and do not affect the long term result of the surgery as long as the skin grafts or flaps do not die.
ReplyDeleteI had my forth surgery on my right underarm June 1st. It was done by a plastic surgeon, but still is not healed...he keeps restitching it about every 15-20 days. After about a week...it looks really good...after the 10 day mark the skin starts ripping where the stitches are.
ReplyDeleteI have confidence in my PS, but I am really getting discouraged. Is this time frame of healing typical...six weeks post surgery...I'm only about 25% healed. I've been visiting your site since my first round of surgery Nov.2011...I see you are dedicated to helping people dealing with HS...
So, I'm hoping you can give me a second, general opinion about the general duration of the healing process for an open wound under the arm after surgery for HS.
Thanks!
Liz
ericlizerickson@gmail.com
Never having seen you and not knowing exactly what was done in your case I cannot make any comments specific to you or your surgery. In general operative sites in HS patients can take a long time to heal and are prone to wound separation and even infection. I put extra retention sutures in because of this. Although that helps it cannot guarantee that you will have no separation of the suture margins. Sometimes it can take 2 to 4 months for everything to heal over. However if your surgeon does a good job of removing the affected areas of skin you should have no further bouts of HS after it heals over. Wounds that repeatedly separate despite suture approximation of the wound edges probably will never heal by suturing and need to heal from the bottom out or are still infected so they will never heal until the infection has entirely cleared.
ReplyDeleteI am scheduled for surgery on my left armpit on Aug 3rd, I also suffer from a less severe form under the left arm and in the groin area, will getting my right arm taken care of increase the severety of the other areas?
ReplyDeleteI would also like to no is there a splint provided post surgery to keep armpit area open
ReplyDeleteEach area of HS is independent of other areas. If you have one area removed it should not affect the risk of HS activation in other areas of the body. That is to say each armpit, groin etc. is affected independently.
ReplyDeleteSplinting is only required if a skin graft is placed. No splinting should be required if local skin flips are used hence the advantage of seeing a plastic surgeon for a flap procedure.
I've been doing som research on surgery options for my HS. Are you fimilar with the CO2 surgery that they conduct at the HS Institute in Ohio? Why isn't this a mor widely used procedure as it's been shown to have very promising results with very little chance for reocurrance and shorter healing times.
ReplyDeleteThere r a lot more places doing it now. The problem I'm told is that this isn't a local anesthesia deal. This is general anesthesia, because they r removing the pores that r believed to be the issue. The best part of this is that u don't end up with uneven, bumpy skin, with giant wholes from where the many matress stiches some inverted and others not. I had surgery in 2012 I was a stage I-II, now I'm a stage I-II all over and it has progressed into other conditions. The jerk surgeon was mad that the ER gave me antibiotics, but they had to because the infection in my armpit was popping my stiches and hurting, and even turning my skin red going over from pit to chest. She said they did flaps everywhere, but didn't close me up with any of these methods in my pit. The Co2 surgery is said to help make sure they find all tunneling. I will now have to do it to pervious groin, buttock, and arm pit. And now the other pit, under breasts, between thighs, and stomach from where I gain all kinds of weight and got it under my belly. I now have some form of acne on my face and neck, and mine is hormone based. They gave me metformin and I was feeling so good, but now they r testing all my hormones, then being put on a testosterone blocker for my pore receptors, and birth control with estrogen because my poly cystic ovaries r causing hormone issues. After that medicine im going to have Co2 surgery to get rid of these sinus tracks I developed.
DeleteAs a physician who performs laser surgery I can say the previous comment is not scientifically sound. There is a large misunderstanding by the general public as to what laser is and can do medically. Part of the problem has been unscrupulous physicians and laser manufacturers convincing the public via advertising and newsmagazine shows (also advertising) that laser is a godsend. Lasers are not some magical star trek device. How a laser works and its effect on tissue are dependent on the type of laser and there are more types or models available everyday. All have in common a collimated beam of light that is absorbed by different tissues with different effects. Some are only absorbed by blood vessels of the skin and leave the overlying skin intact. The carbon dioxide laser is absorbed by water in the tissues and cuts through tissue by burning through it thereby creating "an open wound". The degree of skin injury prior to cutting or along the sides of the cut is dependent on more than one laser parameter. It has been proven at least in rat experiments that if you cut the skin with a laser (with little surrounding skin injury) vs. a scalpel you can't tell the difference between the two incision sites some months later. It has also been shown that laser incisions take longer to heal. Therefore, stitches have to be left in longer to prevent wound separation. So healing times are longer not shorter. Furthermore there recurrence rates are not less because you used the laser. They are less as you remove more apocrine gland containing skin.
ReplyDeleteThe justification that cauterizing with a laser as you cut offers an advantage over scalpels is false. I have seen patients who had
the same hematoma complications after laser eyelid surgery as those who had the procedure performed by sharp metal scalpel.
The belief that there is less trauma with a laser is unfound. Would you rather have an incision that was burned into you with a laser that damages adjacent tissue or cut with sharp cold steel that has virtually no damage to tissue adjacent to the cut?
Hi I was reviewing all the Q&A's and I think I was able to get some what of my concerned answered. I understand you can not give me a definite second opinion but anything counts.
ReplyDeleteI had my hidradenitis surgery 3 weeks ago. Well my surgeon really didn't explain what he did but I'm pretty sure it was the skin flap. Well I have a incision under my right armpit n the top half is closed but there's a two small areas that are still open and at times fluid comes out. He states I am healed in his eyes and I no longer need gauze and antibiotic cream, however I just want to get a opinion if this is normal. Will it eventually close on it's own? I no longer have any stitches.
Thanks
Never having seen you and not knowing exactly what was done at surgery I cannot make any specific comments related to your case. I can say in general that due to the condition of the surrounding skin even after flap surgery separation of some of the sutured skin edges is quite common. That is why I place extra mattress retention sutures at the time of surgery. Although this does not complete prevent separation it does limit the amount of separation. Everyone that has separated eventually healed without recurrence to date.
ReplyDeleteI will be having surgery for my HS in a week. Surgeon said he will be doing surgery with no grafts and it would be for the area where it is recurring. He said he will do for one hand at a time. My concern what exactly is this procedure? will it occur again? Is there any difficulty if i go for both hands at a time?
ReplyDeleteI had been having this problem since 19 years and initially it was oozing but now nothing is coming out from that. I feel like some bone is formed in my armpit. It gets active with pain only. It is recurring twice a month. There are scars for the earlier ones.. But not it is occuring at same spot again and again.
Never having seen you and not knowing what specific surgery you will be having I cannot comment on your case specifically. In general I prefer to operate on all involved areas at one sitting as less operations are better than more operations and the recovery time for all areas can then be combined. I have not found the procedure to hamper range of motion and since there is no need for splinting I see no reason why you would have to operate on one armpit at a time.
ReplyDeleteI find it more disturbing that you are having surgery in a week and do not know what the surgeon is going to do. I cannot see how this would be considered informed consent before surgery. You need to see your surgeon again before next week and not leave his/her office until you understand exactly what surgery he/she is going to perform.
Im an Australian female aged 26 and have suffered from HS for a number of years now, it affects my left armpit, my groin on both sides and a new lump has just appeared under my right armpit leading me to believe it will only be a matter of time before my right armpit will look as hidious as my left one. I have been told by vitually every dr over here that there is no cure and only a select few surgeons will touch it, having read this blog you have given me some new hope that i may be able to rid myself of the hidious disease, my question is are you familiar with any practising Plastic Surgeons in Australia who perform a similar style procedure as you to remove HS?
ReplyDeleteI am sorry I do not know any surgeons in Australia. If you decide to come to Los Angeles I am should be able to help you.
ReplyDeleteI Started out with staph on my legs, when that healed I ended up getting a big soft lump under my arm that begin at the beginning of Feb. By March I had 2 red lumps that were very tender and hurt alot. I have been going to a doctor he has cut both spots but they ust closed and came back. He's not sure if its hidradenitis. Should I get a second opinion?
ReplyDeleteThe leg infection is probably a separate issue depending on where on the leg it was. I have successfully treated hidradenitis of the inner thigh by removing all of the involved tissue. The armpit definitely sounds like hidradenitis. It would presumptuous of me to make a diagnosis without a face to face examination. If you are not confident in your doctor you should get a second opinion.
ReplyDeleteCan cosmetic surgery help with scarring? I have a more mild case of HS but (unsightly) scarring on my buttocks and groin area
ReplyDeleteCosmetic surgery is designed to improve appearance in a normal condition. HS does not fall into that category. I cannot say specifically if your scars could be improved without a face to face examination or photos. Some scars can be surgically improved and others cannot. If you have not had the HS involved areas of skin removed you most likely still have it and treatment of the scars without addressing the HS is moot because the HS will eventually flare up again in those areas.
ReplyDeleteI have lost 134 pounds since I stopped taking steroids for hidradenitis 2yrs ago. I have tried all antibiotics, creams and even humira. I went all natural fruits and veggies no medications and was in remission for a year. I was able to work out and get healthy. Now its back and the loose skin is an issue. Seems to me infection is coming from the extra skin. I can't find a doctor that will remove the excess skin and cut out the hidradenitis. They only want to remove the h.s. but whats the point if the skin is left behind. I'm sure it won't heal. My h.s. is severe it is even in my scalp ( my whole scalp) both arm pit both breasts groin buttocks and my back. I am disabled and on Medicare One surgery at a time seems like years of torture for all those places I don't know what to do. And I don't want to be totally disfigured. I want to live and work again.Will I ever have a nice body and life again? How would you handle this?
ReplyDeleteI am very sorry to hear you are having such difficulties. Your best option is probably to go to the nearest university medical center with a department of plastic surgery. The surgeons in the department should be more than willing to help you.
ReplyDeleteI am going for skin flap surgery on Halloween my surgeon says it will get rid of all the glands. I was wondering how long for recovery (I have a very active 5 year old) and how long after surgery before I can wash the area.
ReplyDeleteThankyou.
If all goes well you should be able to wash the area within 2 or 3 days but uncomplicated complete recovery without any activity restrictions will take 2 to 4 weeks.
ReplyDeleteHi im 27yr old female an i think i suffer from hidradinitis never heard of it an i hav been seen from this but never been told i have it i seen the pictures of it an it looks like my underarm ive had it for a few years an i have been said that laser hair removal would make it go away is this true
ReplyDeleteThere is some anecdotal evidence that laser hair removal helps but it has not helped any of my patients and I have not found any published medical journal articles that describe it as being effective.
ReplyDeleteI had the surgery done on December 18, 2012, it is now January 12,2013, the wound was not covered w/ flaps or grafts. I can feel something pulling in my arm when I try to raise it, the wound is leaking a clear fluid w/ some pus. The doctor did not give me antibiotics. I had to go to emergency for the pain and drainage. I took antibiotics for 7 days, bactrim and keflex, there is still pus as well as swelling around the sutures. What should I do
ReplyDeleteYou are less than a month out from the surgery and should still be under the care of your surgeon. You need to see him or her right away and have them address the issue. I think you will end up needing more surgery to remove all of the affected tissue. If your surgeon cannot or will not help you you can call my office and make an appointment to see me this week.
ReplyDeletehey doc.. i had flap surgery last year on my left side. During the recovery it opened and the surgeon said to let it heal with wet to dry dressings. It only opened on one side of the flap but also the whole bottom kind of popped out so now that everything healed i have the area where the flap tore from the skin and also the bottom sticks out about an inch when my arm is raised and about 2 inches when my arm is down. My surgeon says that he can fix it and tuck the bottom in. In your opinion do these type of problems occur due to poor performance of the surgeon or is it by chance. I am hesitant to do my right arm because of this. Also due to the problems we had my shoulder is messed up sometimes i have pain and my neck feels like it isn't aligned right due to wearing the splint for a long time. Thanx so much for your help.
ReplyDeleteThere are 2 issues here the first being separation of the suture line and the second being shoulder problems attributed to a splint. Never having seen you, not knowing the specifics of your surgery and not know what aftercare you had I cannot make any specific statements relative to your case.
ReplyDeleteSome separation at the edges of the closed flaps/wounds is so common in these cases that it is considered the norm. The infectious process affects the healing capability of surrounding normal tissue so sutures have to stay in longer than normal after surgery and I routinely place extra thicker retention sutures to take the closure tension off of the skin edges. I do not remember ever having to re-operate on a patient just because the edges separated.
I am not sure why you wore a splint since the use of flaps is supposed to enable you to get by without splints. Skin grafts require prolonged splinting to initially allow graft take and later to prevent contraction.
I am also not sure why you did only one armpit. I virtually always do both armpits at the same time unless there are other extenuating circumstances like a very sick patient or no family to help the patient to recover.
I do not know enough specifics to say have the surgeon revise the previous side and do the current side or not.
Thank you so much for your time and response. The reason I am contemplating whether to revise it or not is the aesthetic appearance of the area which separated and the bottom where it hangs.
ReplyDeleteI am not sure why he had me use the splint but he initially said to use it for 10 days post op, but when I returned after about 5 he told me to stop. But once it tore open he instructed me to continue using the splint.
What generally is the recovery for your patients if they do not wear a splint? Can they use their arm normally just no heavy lifting, because my surgeon had me use the splint and I still had problems.
Also the surgeon used stitches that dissolve for the flap I think, and regular ones for the donor area. The surgeon thinks we had problems because my body rejected some of the stitches and they didn't dissolve.
And the donor sight also is not a straight line like the surgeon said. It was at first but then the middle area got all red, it has since gotten smaller and the surgeon says that it is just what the scar is. It looks like this-
---( )--- with the middle space reddish
ps. i believe it was a fasciocutaneous flap pedicled?
Most patients can return to normal activities within 2 to 4 weeks.
ReplyDeleteHi I was diagnosed with HS about two years ago. I stopped wearing deodorant around 6 months ago and it seemed to help a little bit. But now I get this weird smell under my arm, but its not a musty smell as if I need deodorant. I also find that my underarm has a wet moisture like it is leaking a boil..I know it isn't sweat. Any advice/tips? What should I do?
ReplyDeleteYou need to see a doctor who treats HS face to face so you will know how severe the problem is and whether or not surgery is an option.
ReplyDeleteI'm in Philadelphia Pa and I would like to know if you know of any surgeons whom you would recommend.
ReplyDeleteSorry I do not know anyone in your area.
ReplyDeleteHello
ReplyDeleteI have been diagnosis with HS for 6 years now ..I have notice small boils on my buttock,thighs and just recently one in my groin which has been here for 5 weeks now.. it is starting to finally close now. I just started to notice one under my armpit and it feels like its creating a tract.. should I go get it drain ASAP.. I didn't know there was surgery for HS and now I feel hopeful.. praise God.!!! Do know someone one in VA or the east coast you would recommend. I'm desperate and I need help..Ik in the process of getting a divorce and I don't know what to do..I feel so depressed and really need advice. I'm African American is there something I should be concerned about with my skin pigment.
Sorry I do not know anyone in VA. You can call the nearest university hospital department of Plastic Surgery. There should be someone in the department who can take care of you. Draining infected areas can make you more comfortable and temporarily improve things but will not cure the situation.
ReplyDeleteDarker skinned individuals can form worse skin scars so you will need more care after surgery to prevent that than someone with lighter skin pigment.
I have HS. Was diagnosed in May 2012. But i have had it since i had my son 8 years ago. I got pregnany in July and it pretty much laid dormant through my whole pregnancy. Now that i have had my baby...I have a huge flare up. My whole arm down to my elbow was swollen and i was in pain. Tonight it decides to bust and drain. I allowed it to do it's business. Now after its done draining i have a hole in my arm where it drained. Just a tad smaller that a pencil eraser. Is there anything I can do until I get to the doctors next week? Right under the hole it seems to be a pocket of some sorts..odd. When u press the skin underneath the hole it make a hollow noise. Ew!!! I have it covered with bandaids and then wrapped with ace bandage so nothing can get in it. Please...what can I do?
ReplyDeleteNever having seen you and not having a doctor patient relationship with you I cannot make any specific recommendations. In general when you have a surface wound with an associated deeper wound that have been infected you need to clean the wound daily and prevent early healing of the skin edges before the deeper tissues have healed. You need to see your surgeon in order to know if this applies in your case.
ReplyDeleteI went to a general surgeon for a abcess in my armpit that had developed a tract. They did surgery and I had to pack the wound for several weeks. This happened the beginning of February. The wound has healed where its not pack able anymore but the incision has not healed close yet. I can still not where deodorant and its horrible. Should I be worried that its not closed yet? I am borderline diabetic and I know sometimes that can cause issues but I have never had problems healing with anything before. Should I find another doctor because my surgeon is now on medical leave.
ReplyDeleteThat sounds like an incision and drainage for hidradenitis in which case you likely have not seen the last of it. 3 months sounds like a long time to have an open wound which is why it is better to see a plastic surgeon early on in the process. Most surgeons will not close the wound the way a plastic surgeon does.
ReplyDeleteAfter the surgery are your arms completely immobile? Will I need someone available for total assistance with eating, using the restroom, showering etc?
ReplyDeleteAfter this surgery, has a patient's HS resurfaced in the new skin area? Or/also, if all the affected skin is not removed, the HS can remain, but can is spread and "infect" the new skin also?
ReplyDeleteI have seen a few cases where HS appeared at the base of the triangles, where they triangles touch, but this area was small and easily removed. Any remaining HS can form sinus tracts that extend into areas of skin that would otherwise not be affected by the process.
ReplyDeletehello sir i want to know that why plastic surgeons or surgeon do dont completely remove hs affected glands or tissues .are they unable to recognize sometimes to knoe which is infected gland or not?
ReplyDeleteDue to the nature of the disease which frequently involves apocrine sweat glands, the inability to accurately locate all the glands and the possibility that currently unaffected glands may become affected in the future there is no guarantee that all remaining areas of hidradenitis will be removed at any given surgery.
ReplyDeletesir how many apocrine sweat glands are present in armpits is there any exact number or it varies from person to person?
ReplyDeleteIt can vary from person to person and even one arm pit from the other. The number is irrelevant because although apocrine involvement can be seen under the microscope in most cases it is not present in every case. Furthermore, the hallmark of the disease is the formation of sinus tracts not apocrine gland involvement. Although apocrine glands are more numerous in females and in Afro-Americans most of my patients have been caucasian and about half have been female.
ReplyDeleteHello sir my child is 17 and had this condition since she was 14 in both underarms. She used to get it cut and drained which was very painful now shes going through monthly laser treatment to remove hair which we were told was contributing to the problem. She still gets outbreaks every month but it drains on its own after 2 days. Should I start looking for a surgeon and what questions should I ask. Any advice will be appreciated my daughter is depressed about this.
ReplyDeleteAn infected gland was surgically removed from my left armpit about a month ago. Now I have a hole under my armpit after a month. I was told by the doctor that its suppose to heal from the inside. How long does it take for it to heal? I can't see much difference. Thanks.
ReplyDeleteI suspect you had incision and drainage of an infected area which is why it was not sutured closed. If that is the case and you have HS it can take a number of months for the open wound to heal with a high likelihood that the condition will re-occur in another spot in the armpit.
ReplyDeleteHi Aaron
ReplyDeleteMy sister is 21 and has had hidradinitis for almost three years now she has tried all kinds of antibiotics went to doctors and clinics with no joy. she recently started using Dead Sea Mineral Salt Scrub, a product of Deja vu manufactured in Israel. will this help her?
It may provide some relief but it will not solve the problem.
ReplyDeleteSo what do you suggest may help in this case?
ReplyDeleteYou are asking a surgeon for a definitive treatment so the answer is obviously surgical removal of all of the affected tissue. As she is currently finding out, the other treatments are of limited value.
ReplyDeleteI think I have hs. All of these things sound like all the problems im having.It started almost 2 years ago off and on.The smell is so embarrassing. I go see a general surgeon tomorrow. Im sure this is the diagnosis
ReplyDeleteThank you for commenting. I hope you get relief from your treatment.
ReplyDeleteI am a thirty year old female experiencing undiagnosed hs for approximately fifteen years. Both sides of my groin area have been infected leaving scars, black holes (comedones?), discoloration, lumps under the skin, and tracts (almost like they connect). I understand you cannot comment on my specific case, however I was hoping you could elaborate on surgery in the groin area. How do you close the excision? What type of after care is required? Recovery times of 2-4 weeks is understandable, but with surgery in that area are you able to walk, sit, wear clothing? It may sound elementary, but is a "normal" appearance ever achievable after the wound/scar heals? Do skin resurfacing techniques provide any benefit to the appearance? Lastly, thank you so much for taking the time to answer everyone's questions. It really is a relief to know that answers actually exist after years of believing otherwise.
ReplyDeleteGroin is an inaccurate term that we all use. It commonly is used to describe inguinal creases, inner thighs and skin immediately adjacent to the external genitalia. Closure after removal of HS in these areas depends on the specifics of the area involved, wound size and the laxity of adjacent non-HS skin. Therefore 2 people with the same excision may need different types of flaps to close the same wounds. That is why you need to see a plastic surgeon.
ReplyDeleteAbdominoplasty types of surgery can close inguinal wounds. Thigh lift types of procedures can close inguinal or thigh wounds. Thigh or abdominal flaps can be used to close areas adjacent to external genitalia. For all of these you should be able to wear clothing within a week of surgery, walk and sit within 2 weeks and exercise within 4 weeks. These times may be prolonged due to partial separation of flap edges, partial loss of a flap etc. which may or may not need any additional surgery.
The appearance after surgery is highly variable with respect to scars and skin contours. This is not cosmetic surgery. The surgery is designed to get rid of the affected tissue while maintaining normal range of motion, pain free as quickly as possible. If the scars become hypertrophic they can be treated by fractional lasers, medicated tape, scar injections and/or flashlamp lasers to soften or flatten them as needed.
hey I think I have the same thing but all my house is helping giving me some creams and stuff that you haven't really find out what it is but looking at the pictures and looking at this video it is similar as what I have so do I show this video to my doctors so they could tell me if it is or it isn'tso if I do have this so I have to get so you can really I don't want to get scard under my arms but if it's necessary I will cuz this pain is horrible I've been having this since I was 17 I believe and it's not under my my underarms it's also on my private spots and in my side so do you think it is the same thing
ReplyDeleteIt could be the same thing. Ask your doctor if he/she thinks it could be hidradenitis.
ReplyDeleteI'm a 43 year old male who suffers from HS and has for many years I would be what you call an extreme case with boils growing the size of apples about 15 times a year I have tried everything medication wise but I have not found any PS. in Canada who do this procedure do you have out of town patients info that we could look at such as prices and accommodations and recovery time before travel and removal of stitches . I thank you in advance .
ReplyDeleteThank you for your inquiry/comment. Most of my HS patients are from the Los Angeles area, I have had other patients, cosmetic surgery candidates etc, who have come to me in Los Angeles for surgery. You can find accommodations near my office on my website. If you email me your photos I will reply with a detailed price list. You can find an email button in the right column of this blog.
ReplyDeleteI am scheduled to have surgery for hidradenitis on the 20th. The surgeon did say that I will have an open wound because I have enough skin there to close on its own. I am just worried of how I will continue with my work and other daily activities. I am also scheduled to see a wound specialist 5 days after. But I am so worried, nervous and anxious to see some sort of results. The doctor said depending on the soreness of my wound then that's how long it should take for me to return back to work. Can you elaborate more please.
ReplyDeleteNever having seen or examined you I cannot second guess your surgeon or even know whether or not you misunderstood what he/she said.
ReplyDeleteIf there is enough skin there to close on its own why not just close it at surgery and save yourself 3+ months of healing time. This second intention healing is mostly due to contraction of the wound base and not due to the creation of new skin cells to cover the wound. I operated on a patient last week whose wound had contracted down to an inch or 2. With simple thumb pressure it easily tore open to 2 or 3 times that size. I obviously skin grafted the larger wound not the contracted wound. That could just as easily have popped open at home with the patient reaching for something high up in the cupboards.
This is moot when the wound is only an inch or so in diameter because those can fairly quickly contract down. For larger wounds I prefer immediate flap closure or delayed skin grafting. I have left some small ones open depending on where they were located because the tension of closure would have been too great. In some areas of the body second intention healing can cause significant distortion.
I am old school and in my opinion all surgeons should be wound care experts. In my residency I treated thousands of wounds. The current destruction of health care in the US is chopping the care into smaller and smaller bits. The surgery aftercare is included in the surgery fee but if they pay too little for the surgery the surgeon is forced to cut out the after care and pass it on to someone else who then charges for the after care. Pretty soon we will have surgeons who only operate on the left side of the body and another group that only operate on the right side. What healthcare pundits do not understand is that if you pay more people small amounts of money you end up paying more overall in the end and I think end up with inferior healthcare.
Hello!
ReplyDeleteI've been having issues with accesses and such in my armpits, inner thighs, and skin folds for a few years now. I usually end up attempting to drain them myself (which I know I shouldn't, but need the pain relief) because my GP doesn't do it. He has basically told me I get them because I'm obese and that I can't do anything but lose weight and clean them with iodine.
I'm fairly certain my recurring abcesses are HS (of course I'm not a doctor so I could most certainly be wrong). My question is, since my GP isn't being helpful, who do I go to? A dermatologist? I'm not sure who I should go to since my GP is not referring me to anyone.
Thank you in advance for your advice!
I suggest you call your nearest university medical center department of plastic surgery. Tell them what your problem is and make an appointment to be seen. They should have all of the resources necessary to help you out.
ReplyDeleteThank you!
ReplyDeleteI have suffered from hs for 5 years. I just recently had the surgery on the 31st of march. My surgeon did not close my incision v or z flap neither did he do skin draft he sewed my incision back up in the line format, the way that it was shown in the diagram above not to close it back, I was sent home soon as I woke up from my surgery I was an outpatient. I did not have any kind of splint or brace to prop my arm, and prior to my surgery I had a full blown severe outbreak under both arm pits. since surgery my right incision is healing quite well but it slightly bust open and i suffer from so much pain in my right arm, constant burning sensation from the top of my right arm to my elbow, limited movement its very tight and very uncomfortable to move. My left incision just about bust all the way back open my surgeon did not put me on any anti-biotics and my left incision set up an infection, he removed half have the stitches under my right and left arm friday 3/12 and he said that "he was very pleased with the progress of my right arm, but not so much with the left, but despite the infection and open area of the incision it still was healing quite well." I was in so much discomfort sat 3/13 I went to the e.r. and the e.r. dr. put me on antibiotics and was very dis-pleased with the incisions. So I started to do research on the surgery process and the recovery because i was kind of frustrated with the difference of opinion between the e.r. doctor and my surgeon and I ran across this page. Should I be concerned and find another dr./surgeon to take a look at my arms or am i just being paranoid. Your response would be greatly appreciated.
ReplyDeleteNever having seen you and not knowing exactly what was done at surgery I cannot comment specifically on your case. Suture line separation and infections are quite common after surgery for HS. This is outlined extensively in my consents for surgery. To minimize this from happening in my patients I place multiple extra strong vertical mattress sutures at surgery, wash the excision sites with lots of antibiotic solution prior to closure and place my patients on 5 to 7 days of antibiotics that are concentrated in the apocrine glands after surgery. This treatment protocol has worked well in my patients.
DeleteI had surgery done for HS for my right arm pit and my surgeon left the wound open because he said it will heal better and it will heal from the inside out. Is it better to leave an incision open or is it better to sew it up afterwards?
ReplyDeleteThis is called second intention healing. It can work but large areas of second intention healing can take several months to heal in vs. surgery where it is healed right away. Second intention healing takes place mostly by contraction so it can adversely affect range of motion or create webbing. The degree of scarring once all is healed in can be uncontrollable.
DeleteI had a patient in whom I closed an armpit excision with a flap. The end of the flap died so I took her back to the operating room to place a skin graft. In the interim she had healed by contraction. On the operating room table I stretched the healed wound with my fingers and it reopened so I could skin graft it. That scar could have torn open when she was at home reaching for something in a cupboard.
That is why flaps are my first choice for closure and skin grafts are my second choice.
Hey I'm 15 years olds and found these bumps next to my vag and I don't know if its because I shave there or because I work out a lot and don't clean very well down there
ReplyDeleteYou need to see your pediatrician or GP face to face and ask him/her if this could be HS. If it is early treatment is the best option.
DeleteDr. Stone,
ReplyDeleteI have had Hs for 12 years and I am currently at stage 3. I love your responses and I must say that you know your information. I had surgery on 5/28 on my left armpit. All of my armpit had to be cut out leaving a huge wound. I haf a skin flap done which about a week layer started to die. I am going back for surgery on Wednesday to get a skin graft and wound vac put on. Any suggestions for what I can do on my part to help everything go well with the graft?
Flaps can die but despite that they are still the best option for closure in these cases. I do not know the specifics of your case but I personally do not wait a week to do the flap, there is no need to wait. There are only 2 reasons to do the flap at a second operation.
DeleteThe first is insurance reimbursement i.e. charge once for the excision and a second time for the flap. If you do them together insurance only pays for the flap.
The second is if you are worried about blood supply to the flap in which case you delay it. At the first surgery you excise the HS and partially raise the flap. At the second you raise the flap completely and swing it into place.
I had a patient on whom I did excision of both armpits and under the breasts with flap closure of all areas at one operation. I tried to ultrasound the arteries to the armpit flaps before surgery but could not find the signals. The armpit flaps were basically the same on both sides but the distal half of the flap on one side died. The only explanation I can think of was the patient slept on that side and kinked the blood vessel. I debrided the dead area in the office and then went back to place a skin graft, which was much smaller than what would have been required without a flap.
The best thing you can do to help the skin graft survive is keep the area immobile for 10 to 14 days. All the other factors such as adequate bed for graft survival, absence of blood under the graft etc are in the hands of your surgeon.
Hello Dr. Stone,
ReplyDeleteI am a 32 yr old female who has suffered from HS for about 10 yrs. It started on my bikini line,which, thankfully, has not reoccured in a couple of years. My first question would be, could I have another HS flare in that area after not having any issues in a few years?
Unfortunately, I now suffer from HS under my R arm in the armpit. I have had 3 drains done by an ER doctor and now, I have a permanant sinus drain. It simply will not close. I know the only solution is to undergo HS surgery. I will definitely be looking for qualified Plastic Surgeons in my area.
My next question is, Why do the majority of physicians clain this to be a "clogged hair follicle?" This annoying DX has been given to me by many many doctors. The solution, to them, is always Keflex and to stop shaving. Unfortunately, I found tat shaving does seem to aggrivate my HS and ultimately cause a flare. Is this just coincidence?
Thank you for your time. I truly wish the world were full of physicians as dedicated and pleasant as yourself.
Sincerely,
Crystal R.
Any HS involved area that is quiescent can flare up at any time even if it has been some years since the last flare up. Early HS is hard to discern from other skin infections like folliculitis. It is not until you have multiple active areas or develop scarred sinus tracts that the clinical diagnosis becomes clear. Shaving can cause armpit HS to flare up but so can sweating after working out.
Deletehi dr aron
ReplyDeletei have hs stage 2 in both axilla my dermatologist said me to have wide radical surgery in both armpits but my plastic surgeon dont know about hs and he has never done surgery for this but he is best plastic surgeon in country pakistan so should i get operated by him or not?
I do not know the specifics of your case and do not know the surgeon so I cannot say whether or not he/she should do your surgery. The important factors are your comfort with the surgeon and his/her comfort/skill in raising the necessary flaps to close the wound. The number of HS cases this surgeon has treated is not as important as their familiarity with parascapular and fasciocutaneous flaps would be.
Deletehi dr aoron
ReplyDeleteis this hs disease is present in superficial skin or deep down in fat tissues something like that as i have read on many sites that disease dwells inside deep fats hidden apocrine sweat gland .if any single infected apocrine sweat gland is left inside and not removed then hs can come back and how deep PS has to dig into armpit to get rid of entire infection.
It is a skin only disease but in chronic cases with superimposed infections the infections can spread down into the fat or even the muscle. I had a patient who had such advanced armpit disease that at the time of surgery I found it it extended into his chest muscle and I had to remove some of the pectoralis major chest muscle.
Deletethanks for information doctor you are really doing great job serving humanity we all hs sufferer are so tense..
ReplyDeletehi dr
ReplyDeletewhat are the factors due to which hs reoccur even after surgery and i heard from few people that they got surgery of axilla and their axilla problem cured but hs started in other anotomical areas of body like groin or buttocks is there any connected of surgery with other parts..please guide if u can so that we can care about those factors while having surgeries..THANKS
If you have hs it can pop up in any susceptible area of the body. Having surgery on one area alone does not impact the hs in other areas of the body. If you have surgery in one area and have a complication such as an infection that could aggravate hs in other areas of the body but that is a separate issue. If you need surgery in one area you should not avoid the surgery for fear of activating it in other areas.
DeleteHello Dr.
ReplyDeleteThis sounds exactly what I have been suffering with for a while now. For years I have had the lumps that show up and eventually drain then heal up. A while ago I had one under my left arm that just wouldn't heal up. It stayed small for a long time and now it has gotten larger and larger until it takes up most of my armpit. It is extremely painful and the drainage is horrible. My big problem right now is I am unemployed and have no insurance. if I go to the ER will they know what this is and do you think I would be treated. I am about at the end of my rope with the pain and draining. Thanks for any info or suggestions you may have.
Option 1 if you are on food stamps have them sign you up for Medicaid. Option 2 go to your state's obamacare website and sign up for a subsidized plan. Either way it will be tough to find someone to take care of you. Option 3 contact your nearest teaching hospital and enroll in one of their programs for the poor and uninsured.
DeleteDr. Stone,
ReplyDeleteMy 18 yr old daughter has this disease. She has already had one surgery and is now looking at having surgery number 2. She has also had a boil come up between her breasts, in which they lanced. The surgeon states she is going to need a skin graft this time. She starts back to college soon and I am worried about the recovery period with having a skin graft. Should I mention the skin flap to the plastic surgeon? Is this a better option as far as recovery?
Never having seen your daughter I cannot comment on the specifics of her case. I have removed HS between the breasts and directly closed the wounds. I have removed some and let them heal in on their own. I don't remember ever placing a skin graft between the breasts after HS excision. In general I prefer flaps to grafts but I have done both. It depends on the patient and the area to be closed.
DeleteHello Dr Stone,
ReplyDeleteLast 31st August, I had undergone a surgery for HS on both my armpits. Surgeon advised me not to wash both armpit areas until the removal of my sutures which would be after 10 days. After some periodical dressing changes (1st Sep, 5th Sep, 8th Sep) I visited my surgeon on 11th Sep to remove my stitches. Previously when I was changing dressings these wound were healing without infections. But on 11th he removed stitches from my right but my left armpit had a opening hence he took me again in to the operation theatre and re stitched it & put up a dressing to my right armpit just for the sake of safety. After another 3 days which he asked me to come & show him the condition of the wounds my right one has also been opened and both wounds looked draining with pus like serum, even the left armpit which he just re stitch 3 days ago. Then he said he will have to put the stitches again to close the right one and explained to me this was rare & sometimes this kind of things can happen. So after 14 days of the surgery, its like these wounds became just as new like they were after the operation. I mean I asked him what if this happend again when Im coming after 14 days to remove sutures. He explained it will not happen again to me. And also I have been following post surgical instructions he gave to me up to now and was taking antibiotics 3 times a day from the day I had the surgery (Amoxicillin 500 + Clavulanic 125). As of today (18th Sep) I dont have that much pain unless I tried to move my arms in wide arcs. Sometimes I fear this might take forever to heal and also Im loosing faith in my surgeon as well.
Dr. Is this condition normal in your opinion or is it that he is not telling me something that has gone wrong ???
Thank you very much in advance
Not knowing the specifics of your case or surgery I cannot comment specifically about your surgery or if anything has gone wrong. In general I have all patients bathe beginning 2 or 3 days after surgery to lower skin surface bacterial counts but different surgeons have different preferences. Healing after HS surgery is never straight forward because the surrounding skin that is not directly involved with HS is not normal skin. Whether I do a flap, direct or complex closure after HS excision I always vigorously wash the area with antibiotic solution in the operating room before closure and close with large retention sutures. Together with a short course of antibiotics after surgery I have found that the problems you describe are minimized but never removed from the equation. High tension closure without a flap in these cases will not stay closed.
Deletehello what's your opinion on using a CO2 laser to remove hidradenitis? There is this Dermatologist that uses the procedure. The patients that have gone to him have minimum to no scarring, the chances of hidradenitis was lower, no stitches were needed and the patients returned to their regular everyday lives afterwards. With this surgical procedure i have been told by surgeons its extremely painful, it takes weeks to heal, and patients had to come back to have surgery years down the line. I also need a breast reduction. If it's only in my armpits would it be a good idea to get my breast reduction then work my armpits later?
ReplyDeleteYour questions are excellent.
DeleteIf you use the fractional CO2 laser you will have no down time, no raw surface areas and no scarring from the laser. In the process you allow the affected areas to drain through the skin and soften/flatten the visible ridges in more advanced disease. However, you will not cure the condition and at some point in time it will have to come back. If you use the non-fractional CO2 laser you will have raw areas that will need suturing, flap closure or skin grafting.
Armpit hidradenitis in someone who needs breast reduction surgery is tricky. If you cut out the HS and want to close it with a flap you cannot use the double opposing V-Y flaps described above if you do the breasts and armpits at the same operation. The skin closure during the second part of the procedure will be too tight. Moving the breast skin, that would otherwise be removed, into the armpits would irreparably damage the architectural proportions of the breast. If you do the armpits first with the double opposing V-Y closure you will be able to get the same breast reduction some months later with a smaller skin excision and therefore a smaller skin incision/scar.
When I put "with this surgical procedure", I was referring to the skin flap /skin graft surgery
ReplyDeleteHi i have hs i was diagnosed a couple months ago but have had the symptoms for about 2yrs its to the point where my flesh is hanging out of my arm. Its so painful wen i touch it it bleeds and i have a very hard time lifting my arm. Would it be best just to get surgery or go to a dermatologist first? I have an appt with one i just feel like im too far gone with this
ReplyDeleteNever having seen you I cannot tell you what to do or recommend a specific treatment. Surgery sounds like it may be a better option but the dermatologist should know better after seeing you.
DeleteWhat procedure might be done if you have hs under your gut(sagging stomach) and panty line area plus on and around your vagina?
ReplyDeleteThe ways I have treated this in the past after excision were to use the skin that is usually removed as part of an abdominoplasty or thigh lift to close the wound. You can also rotate a flap of skin and fat from the thighs into the area to close the wound. These modalities give the patient a quicker return to normal activities and less chance of restricting motion of the limbs/body than allowing the wound to heal on its own or skin grafting it.
DeleteThanks. I was told today by PS that I need a mastectomy for my HS on and under my breast. Is this necessary? I'm so hurt hearing that.
ReplyDeleteThe process involves the skin so you have to remove the skin only. In some cases the process invades deeper tissue so you have to remove that tissue as well but I find it hard to believe it would affect an entire breast necessitating a mastectomy. The question is how do you close the resulting wound. The surgeon you saw may be trying to take the easy way out by just removing the breast. The better alternatives are mastopexy, pedicled thoracodorsal artery flap, breast reduction and skin grafting in that order of preference. I suggest you get a second opinion as I doubt a mastectomy is necessary.
DeleteWhat kind of surgery would you call this though? Or what type of doctor does this surgery for my armpit? I had it lanced about 4 years ago... But it is back. I cannot wear deoderant and I am scared to shave. This is so painful
ReplyDeletePlastic Surgery performed by a Plastic Surgeon.
DeleteI have this! its been going on and off almost 2 years now its very painfull first it was the right armpit and the hole finally healed but still fills, now its the left one and there are two holes and out of the bigger hole its draining yellow and for awhile was smelling pretty bad, I been using a&d ointment and the smell has gone but still leaking here and there yellow im terrified to have surgery but its most likely in my future what happens if its not taken care of ????
ReplyDeleteYou may be able to control it medically such as with newer immunologic medications but you can only cure it by removing all of the involved tissue. If you do nothing and let it run its natural course the infectious process can invade underlying or adjacent normal tissue. I had a patient whose HMO refused to operate or do anything definitive for decades. When I finally operated on him the process had begun eating into his chest muscles and I had to remove part of the muscle on one side. That was a shame because it starts out as a superficial process only involving skin and only requiring removal of that skin.
DeleteHi. I have HS in the groin area and underarms. My dermatologist said surgery might be good for it. My question is if a plastic surgeon could use the excess skin on my thighs to close the wound, basically giving me a tight lift? Would most insurance cover that?
ReplyDeleteWithout having seen or examined you I cannot say for sure but the answer is probably yes for the surgery and yes for the insurance within the parameters of their in and out of network policies.
DeleteAm suffering from this.. Doctors prescribed me some antibiotics and I used them for almost a month but there is no change doctor asked me to prefer surgeon to take surgery but I refused because currently am taking few exams and I don't want to get disturbed but day by day it's getting worse what should I do? I can't take surgery because of board exams? Is this surgery very painful? should I prefer plastic surgeon or general surgeon?
ReplyDeletePlease reply soon
As you are aware antibiotics are not the answer. I recommend you see a plastic surgeon now and prepare for surgery after your exams.
DeleteHi Dr. I wanted to know what kind of surgery would be performed for hidradenitissuppurativa in creases of thighs? As well as on top of and inside vagina?
ReplyDeleteThat would depend on the size of the defect after the hidradenitis affected tissue is removed and the degree of laxity in the surrounding skin. The closure flaps can come from the inner thigh (gracilis), outer thigh (tensor fascia lata), the entire thigh (thigh lift), the front of the thigh (anterolateral thigh flap), the abdomen (tummy tuck skin that is usually discarded). No 2 cases are exactly the same so the surgical plan is different for each patient.
DeleteHi Dr.
ReplyDeleteI recently had HS surgery under my armpit and the doctor left it open to heal from the inside. But, there is a drainage of clear to slightly tinted yellow fluid coming out and it smells horrible. To me it smells like necrotic flesh or something but there is not infection. The doctor said there may be drainage of clear fluid but this is unbearable with the smell.
I hear there is a lymph node in the area so is it possible the drainage could be the lymphatic fluids or something? Or could it just be the sweat gland but what about the smell?
Is there anything I should ask my doctor in particular or anything you can suggest I do to try and stop the smell until my next doctor's visit? It was done about 2 weeks ago and the incision is from front to back under my armpit right where the arm meets the side in the bend. He stitched it up inside but said he was leaving it open on the outside to bandage and allow to drain. Bandaging the area as you know is all but impossible, though, and I spend more time changing bandages than I think necessary...about 5 times a day right now.
What i'm concerned is the smell mostly. It's not a sweaty smell of armpit or anything. Its almost like something dead, to me at least. And the scent is so bad I do not want to be around anyone, and it even makes me sick to my stomach smelling it pretty much 24/7.
Any advice/information I can use or ask my doctor? I'm at wits end dealing with this smell.
Thanks.
Never having seen you or your wound and not knowing exactly what surgery was done I cannot make specific comments. Open wounds usually have an odor because of infection or dead tissue. There are a number of topical ways to deal with these problems including surgery to remove dead tissue, topical medications to dissolve dead tissue, topical impregnated dressings to absorb drainage and kill bacteria etc. You need to have a frank discussion with your surgeon whether he/she needs to remove more tissue, apply a specific dressing or if you need a second opinion. Second opinions are best given face to face knowing all of the facts rather than in a blog format.
DeleteHow long is recovery? What are some of the side effects from getting this procedure done bilaterally? I have to see a plastic surgeon on 06/11 & hoping he does this procedure before I start school on 07/14. How can I help expedite my healing?
ReplyDeleteThe major side effect is you no longer perspire as you usually would from the armpit area. As with any operation there is a risk of complications. If you have a smooth recovery it should take 2 to 4 weeks. If your recovery is problematic it could take 4 to 8 weeks. The best way to expedite healing is to follow the instructions of your surgeon before and after surgery.
DeleteHi I have to have hs surgery on my left armpit and I was wondering if it's a wise decision to have liposuction done on my arms at the same time.. kill two birds with one stone... And also I've been told that it will be cheaper to pay for the liposuction because my medical will already be covering most of the cost from the hs surgery. Is this true
ReplyDeleteI gather you feel there may be something wrong with this which is why you are asking the question. There is something wrong with this because your bloodstream will be seeded with bacteria during the HS surgery and obviously some will end up in the liposuction area. Furthermore, liposuction is best performed by passing the cannulas in more than one direction. For the arms this usually means access sites in the armpits and at the elbow. That means the cannula will also be directly passing bacteria into the area of liposuction, not a good idea.
DeleteCombining insurance covered procedures with uncovered cosmetic procedures in the same operation is tricky. Anesthesia and facility billing have to clearly separate the time involved for the covered and uncovered portions of the surgery. The insurance companies do not want to cover any of the costs of any uncovered cosmetic procedure. So they will NOT "be covering most of the cost from the hs surgery".
Hi, I am almost 100 percent sure that I have HS but I am nervous about what I should do about it. Right now, it is in a good period but when it is bad-it gets super swollen and painful, and maa burst and leak. It is not jusmp one lump but multiple ones all in my left armpit. It has gotten up to 3 spots that are leaking at once and now once hole wont close. When I raise my arm there is a hole that you can see into my inner tissue. I did see my doc for it who said it was probably folliculitis and sent me to the surgeon...the surgeon did not believe it was folliculitis and told me to wait until it flares up again and then come back for him to see it personally (that was before I got the hole). Anyway, as long as it is what I will call-in remission- or not bothering me really. is it safe to kinda forget about it? Also should I be doing something to the hole?
ReplyDeleteNever having seen you face to face I cannot make specific recommendations or even a diagnosis. HS characteristically waxes and wanes in terms of its activity. Ignoring it when it is less active is not a good idea because it is at some point going to become active. If you go the route of surgery it is certainly easier to remove and there are less complications after surgery when performed on less active HS. Biologics certainly are more effective when the HS is less active. I hope this helps you make a decision.
DeleteThanks for your response! I guess I know i should go back but i'm sooo tired of doctors at this point lol. I was just hoping I could put some neosporin on the hole and it would close and my life could go back to normal :)
ReplyDeleteSorry to say so but that is unlikely.
DeleteWhat about people who are highly allergic to sutures of any kind? I was very recently diagnosed with this and am terrified.
ReplyDeleteI can't have sutures.
I have seen this problem in other patients. We now have sutures made from so many different substances that it is impossible to be allergic to every single one. Nylon and Prolene are so inert that they are used to repair arteries. Usually it is the absorbable like Vicryl, PDS etc. sutures that people have problems with. Most of those patients do well with Chromic sutures or just no absorbable sutures at all.
DeleteHi, I had HS surgery under both arm pits on February 15....recovery is good thus far. I think I pulled a stitch loose, hence mre drainage than normal. I go for a follow visit on the 25th. Im kinda scared to move my left arm in fear of more stitches popping. I have this tenderness, weakness and numbness in that arm. Woild it be safe to do light arm excercise to regain some strength
ReplyDeleteIt would not be proper for me to give you postoperative instructions after another surgeon did your surgery. If this cannot wait until your next visit you should call his/her office and speak to someone in that office as soon as possible. You should feel comfortable doing so because the payment for surgery included the care after surgery and when you chose your surgeon you should have chosen one that you feel comfortable with, one who will do competent surgery and be there for when needed after surgery. The government and the insurance companies want to take away your right to chose a surgeon and hopefully that did not happen to you.
DeleteI have a hole in my armpit for almost six months now and it does not seem like it is healing... What can I do to help it to heal
ReplyDeleteNever having seen you I do not know what your problem exactly is. If it is hidradenitis your best option is to see a qualified surgery not to help it heal because it will not heal on its own.
DeleteI had surgery on my left armpit about 12 years ago and within the past several week I have noticed swelling around incision site/scar. It is quite painful and I am a bit confused and concerned. Any ideas?
ReplyDeleteThis could be anything from a furuncle to hidradenitis. You should be seen face to face by a surgeon sooner rather than later in order to know what the problem is and how it should be addressed.
DeleteI am having both my axilla excised in February. I am very nervous about the surgery reducing range of motion permanently, can you please advise likelihood of this happening? I'm not sure my surgeon is being fully upfront about the issue. Also, will I need to wear deodorant afterwards? Supposedly all the sweat glands are being removed so I shouldn't be sweating/smelling afterwards. I know you can say for sure, but if you've gotten feedback from your patients about this I'd like to know. Thanks
ReplyDeleteThe final range of motion depends on how you heal and how the wound is closed, which are both unknown to me. You should not need deodorant afterward if the excision is adequate.
DeleteI still needed deodorant afterwards. Not to stop sweating, but because it still smells like an armpit.
DeleteI have HS in the groin area and around the butt as well as both my armpits. In one armpit I have little to no scaring and currently have no 'boils' /cysts. I have seen doctors about this and want surgery. You are the only person I can find that knows a lot about this. Unfortunately. I live in Canada and don't know how I could get the surgery by you. I am 19 years old. I believe I am stage 1 in some areas and stage 2 in the groin area. I also had some questions:
ReplyDelete1.For the groin area, where will you be taking the extra skin needed from? My thighs?
2. Have any of your patients, after having this surgery (that is uploaded on your youtube) got HS back? Or are they all cured forever after surgery.
3. Does shaving cause of worsen HS?
4. Can food have an effect on this? I read some articles of people saying that when they changed their diet they stopped getting HS boils etc.
5. Will I ever get HS again if I get the surgery from you?
6. Does this surgery (the one on your youtube) remove aprocine glands? And if so, will I sweat if I have them removed?
7. Some people say they get HS back after surgery, but if HS is in the aprocine glands and those glands are removed then how can people still get HS?
Thank you so much! I would really like for you to do my surgery I was not able to find a doctor who knows a lot about this as you do. I am not sure if my Medical would cover out of country surgery. Thanks again!
1. For inguinal fold areas the skin comes from the adjacent abdomen and/or thighs akin to a thigh lift or tummy tuck. For perineum/genital area a flap may be rotated over from the inner thigh or upper back of the thigh.
Delete2. None of my patients have had a recurrence in an area that was excised.
3. Shaving does not cause or worsen HS though hair removal by laser may help the condition.
4. Food has no effect on HS.
5. You could get HS in an area adjacent to the excised area or if you have it in the groin area you could develop it in the armpits at a later date.
6. If you have surgery in the armpit area you will no longer sweat armpit type of sweat but all normal skin does sweat as do any flaps of skin used to close a wound.
7. They either developed it in an area adjacent to the excision, did not have a full excision or they had an incision and drainage i.e. inadequate surgery.
Canadian government health insurance does not pay for non-emergent healthcare delivered outside of the country. I hope this is of some help to you and I would be happy to be your surgeon if you are able to come to Los Angeles.
How much would surgery cost (approximately
ReplyDelete)in USD with no medical insurance help if I wanted the surgery in the groin area and both armpits by you. I am stage 1/stage 2.
That cost depends on the size of the defect after removal of the tissue and the size of flaps used to close it. If the site can be closed without flaps by just undermining the surrounding tissue the cost is significantly less.
DeleteDr Stone, I have been suffering with HS for many years. I am currently suffering with one large under my armpit with now scarring and tunnel it is discharging every day for the last 6 months with two months of that was during the end of my pregnancy. My son is now 4 months old. I also have two in my groin area have already discharged and drying to heal but currently still sore as I'm having difficulty in dressing both areas due to me being quite hairy.Both areas are quite painful but my doctors doesn't seem to be doing much other than giving me flucloxacillin which I've had 4 courses already and hibiscrub Wash. Nothing's working and I'm getting very down. Should I push for surgery? I am scared as I have the baby who I am breastfeeding. I don't know what to do.
ReplyDeleteI would recommend the surgery but it might be best to wait until you can take a break from breast feeding for a week or so in order to clear the anesthesia and pain medication from your system. Good luck and congratulations on the birth of your son.
DeleteThank you very much. I will do that as I plant to put him on formula milk from 6 months of age. Should I request to see a plastic surgeon?
Deleteyes you should
ReplyDeleteDr. Stone, my granddaughter is 16 and currently has this condition. She is in a very active phase of it right now. I believe it is inherited as her father and paternal grandmother have it as well. She has been treated for the last year with antibiotics for it and it has provided no relief or results. The purse inside of the boil tested positive for MRSA. She was admitted to Halifax Hospital because of the MRS a. The plastic surgeon saw her and told her that she absolutely needed the procedure that you detail done and that he would be willing to do it but first the general surgeon needed to drain the boils as she has about seven active under one arm and I don’t know how many on the other not as many. When they did the ultrasound they could see the tracks underneath the skin and all of it running together. They scheduled her for surgery and the general came to see her look at the ultrasound and then decided that he felt the surgery was out of his scope because she was 16 years old. Now they are going to either discharge her with anabiotic’s or try to find a pediatric hospital that will drain the boils. My questions are as follows:
ReplyDelete1. Is it necessary to drain the boils prior to doing the surgery taking out the lymph node and the sweat glands and re-creating the armpit?
2. Should they continue treating it with anabiotic as when I read your paper it said that that can lead to cancer situations if treated that way over multiple years?
3: my granddaughter lives in Daytona Beach Florida can you recommend or is there a website of some kind that we can find doctors that are from Milyer with this condition in her area? That area would go from Jacksonville to Orlando Florida?
Any thoughts or recommendations or answers that you can give would be greatly appreciated thank you. Sincerely Maureen Oudt
The best case scenario is to do the definitive surgery at the first operation but that is not always possible if the disease is active with pus and antibiotic resistant bacteria. The reason is that when active adjacent non-HS skin is not normal and though it does not need to be removed it does not heal normally. The options are to either first acquiesce the HS or do a 2 stage surgery. Aquiesce could mean aspirating with a needle and syringe, performing an incision and drainage etc. In your granddaughter's case it sounds like the plastic surgeon did not want to do the first stage and instead wanted the general surgeon to do it. The general surgeon then got cold feet and wanted to turf the case to a pediatric surgeon either because he/she did not want to do it or his/her hospital does neet treat children/adolescents. I don't see why the surgeon who closes the wound can't create it by removing the involved tissue either as a 1 or 2 stage procedure. Sadly this could be related to your health insurance and its fee schedules to physicians.
DeleteI can't recommend any specific surgeon or hospital in Florida as I am located in California. Her best remaining option may be to contact the plastic surgery department at the nearest university hospital, likely in Tampa or Miami. Surgeons in the department should be able to perform whatever surgery she needs.
Is the use of this surgery to treat very bad body odor successful? I tried Sweat gland suction and Miradray but no improvement.
ReplyDeleteThis surgery is a bit extreme for that problem. If miradry did not work autonomic nerve surgery or removal of the glands via multiple parallel armpit incions is a better option. I don't know the specifics of your surgery but it may have been inadequate for technical reasons.
DeleteAre there doctors or hospitals
DeleteHave this surgery ?( removal of the glands via multiple parallel armpit incions)
in Europe or Middle East?
I do not know but I would hope so.
DeleteAre there antiobiotcs you can buy without a prescription that may work? Also is a good idea to put antibacterial cream on them. Had MS for about a year scared for surgery bc no definite it won't come back
ReplyDeleteIn the US antibiotics can only be obtained by prescription and this is important to restrain the number of bacteria that are resistant to antibiotics. You can get topical antibiotics over the counter but these are of limited use in active infections other than folliculitis. I don't believe topical antibiotics are of much use in HS. I can understand your reluctance to undergo surgery as there are no guarantees and I assume you meant HS instead of MS. However, I think most patients that have definitive surgery are glad that they made that choice. Your best bet would be to speak to people that had/have your degree and location of HS and have had or decided to forgo surgery. I think the relief that comes with being disease free for some years is well worth the effort.
DeleteHi Dr Stone, I had a HS surgery on my right armpit. After a week when my stitches took out that looks fine. Nurse gave me some dressing to changed everyday. It was fine up to 11 days of my surgery but after that I found my wound was opening. And drain smelly fluid types something. I went to the hospital where I had surgery Nurse seen the wound and said because of moist it was open and wound takes time to heal 2 to 3 weeks. So she puts again dressing and said not to open 2days. After 2 days when I went to see my GP nurse I saw few of my stitches area getting open wider and I can see the pink skin. And also that area draining pus now. My question is stitches was fine after taking out the bandages. But now few place of stitches why looks pinkies. Is that normal? Now I am using small dressing just under my wound. Other side of stitches are leave it open my GP nurse told me to do that. Am I doing right?? Thank you in advance
ReplyDeleteI leave sutures in place after HS surgery for as long as 2 weeks because the skin in these patients takes longer to heal. The most common complication of HS surgery is separation of the suture lines. As long as the excision was adequate these heal with time. I am more concerned that you are seeing nurses only instead of your surgeon. That is not the norm in my practice.
DeleteHi Dr Stone, at first thanks for ur reply. My surgeon will seen me after 7/8 weeks but in the main time if Nurse found any complication she will refer me to the surgeon. Otherwise I have to visiting my GP Nurse twice a week.
ReplyDeleteHello, thank you for answering our questions . I'm 31 & a female . I think I've had hs for about 3 years now. I haven't been diagnosed by a doctor yet but I pretty much diagnosed myself after doing a ton of research online . It started when I was pregnant with my now 2 1/2 year old. At first there was a strain in my right arm when I reached my arm out . Then the bump formed . It darined slowly started to form a tract then healed . I haven't had a problem in the right arm pit since. But the left armpit I believe is in stage 2. I've seen pictures and it looks like stage two . There is a for sure a tract which had several small pin size holes that slowly drain smelly puss. Very very very painful at times it can be hard to move the arm all together . I seen a few doctors that automatically said they were just boils or mersa without testing anything . I even swabbed it myself when I first was seen early in my pregnancy but they didn't test it and automatically said it was mersa. ( think that's how you spell it ) so I never received any treatment or antibiotics for this condition ever . I went to the er about a year ago and they just wanted to cut it open but couldn't because the cyst was too hard and again passed it off as mersa . So I got dicouraged and started doing my own research and have been using natural remedies. Turmeric vitamin c & tea tree oil seem to help keep them down a lot . also im trying to wat healthier as a study showed brewers yeast may be a big contributing factor hs . I've read up on the whole 30 diet and though about trying it to see if that eliminates this horrible hs. Not sure what your thoughts are on lifestyle changes such a healthy eating and its effects if any. The turmeric and tea tree oil realky help some days i dont even feel the effects of hs . i also use witch hazel to help clean the area But I know it's not a cure and the last few weeks it's not really helping. the tract under my left arm is inflammed it drained on its own a little after I put scolding hot water on it, only when I put scolding hot water for two days do they begin to drain . My question is how do I know which surgery to get ? I know I probably need the surgery. Even tho I'm scared I will do it if it will help . there is a tract and it's active ...flair up , it's draining slowly. What do you suggest I do next ... call a dermatologist or a plastic sergon? co2 surgery or no ? Which surgery is the most effective with the conditions i just described ? this might be the scariest thing i encounter besides having kids but if you think it will work I trust your experience. Thank you so much for your time .
ReplyDeleteHS gets better and worse on its own so affected individuals often attribute a diet or treatment as being beneficial when it really is not. The surgery to get is the one that removes all of the affected tissue and allows for the quickest healed recovery. The surgeon best equipped to do it is a plastic surgeon. The use of a CO2 laser adds little or nothing to the process because you still have to remove the tissue, send the specimen to pathology and close the wound. If you destroy the specimen with a laser you are left with something the pathologist cannot examine.
DeleteMy twins father has H.S. he had been in a nursing home for two years in Califorinia. He has been suffering with open wounds for over 3 years now he is 46 and in desperate need of help do you have any suggestions please help...he is now at the point where he hasn't gotten out of bed on his own without assistance and he now has a pressure point on his rear from just laying in bed dealing with embarable pain...any suggestions...please help.
ReplyDeleteHis problems will require care by more than just a plastic surgeon. His best option is to contact the nearest University hospital department of plastic surgery to arrange for a consultation with the required specialists and likely initial inpatient care.
Delete